Public health responses to increases in mosquito-borne viruses, such as chikungunya, dengue, and recently the Zika virus outbreak, have increased awareness about these illnesses. This is especially so with the Zika virus and its devastating effects on unborn children. Awareness and prevention guides are now more widely available. However, information provided is often limited to telling consumers what to do to protect themselves from mosquito bites, lacking an explanation about the cycle of transmission in a simple and concise way. Better understanding about why protection is critical, and how this action protects others, may lead to more consistent protective behaviors. Nurses interact with patients on a daily basis and are trained to convey complex scientific and medical information in ways that are understandable to different populations. For this reason, nurses are critical partners to teach about prevention and control of mosquito-borne illnesses. This article will first briefly review arboviruses, followed by an exemplar that discusses customized teaching tools about dengue fever developed for lay persons traveling for mission trips. The summary offers recommendations for nurses to consider as they plan intervention to increase awareness and prevent and control outbreaks.
Keywords: mosquitoes, viruses, mosquito-borne illnesses, education, vector ecology, pathogen transmission, Chikungunya, dengue fever, West Nile virus, yellow fever, Zika
There is a worldwide increase in the spread of mosquito-borne viruses... Mosquito-borne viruses are becoming more prevalent in and near the United States (US), and Americans are paying attention (Woerner, 2013). There is a worldwide increase in the spread of mosquito-borne viruses that cause illnesses such as chikungunya (CDC, 2016a), dengue (Bouri et al., 2012; Van Dodewaard & Richards, 2015), West Nile virus and yellow fever, and Zika (CDC, 2016b). These five viruses cause clinically similar symptoms.
Patient education, symptomatic treatment, and vector control are currently the primary focus of care management. There is a vaccine for yellow fever. Over the past two years, vaccine development has progressed for the chikungunya, dengue fever, West Nile, and Zika viruses (Fogarty International Center, 2016; National Institute of Allergy and Infectious Diseases [NIH], 2016, 2015; Roos, 2015; World Health Organization [WHO], 2016b). Nurses are trusted health professionals in a unique position to influence awareness and education about vector ecology, transmission, and clinical characteristics of these diseases in ways that are easily understood to help reduce mosquito-borne transmission and control growing epidemics.
...most materials tell readers what to do to protect themselves from mosquito bites, but do not always fully explain the cycle of transmission. With increasing interest, information and guidelines are becoming widely available. However, most materials tell readers what to do to protect themselves from mosquito bites, but do not always fully explain the cycle of transmission. As such, this information may not teach the importance of preventing mosquito-borne illnesses (CDC, 2016c, 2016d, 2016e) and does not always lead to sustained behavior change (i.e., consistent protective behaviors) in the population. An explanation that explains why, provided in a simple and concise way, can help populations at risk to better understand the need to protect themselves and also how this action helps to protect others.
Nurses are educated to convey scientific and medical information in ways that are understandable to different populations. Nurses are educated to convey scientific and medical information in ways that are understandable to different populations. Providing nurses with information and plain language tools to teach populations with whom they interact about the complex living cycles and relationships of mosquito-borne illnesses is essential. Each nurse, as a behavior role model, can have a pivotal role in teaching the transmission cycle, vector ecology, and disease manifestations of mosquito-borne viruses.
Nurses must first understand the why of mosquito prevention to actively engage using education, outreach, and graphic tools as a basis for prevention and behavior change. Nurses need a basic understanding of the complex vector ecology of the arboviral diseases, and how the viruses are transmitted or ‘borne’ in the gut of mosquito arthropod vectors. This increased understanding will provide foundational information for nurses as they explain to people the importance of protection from mosquito bites at all times.
The first section of this article will provide a brief background about arboviruses and review vector ecology, pathogen transmission, clinical manifestations, diagnosis, and prevention and vector control. Tables and figures provided in this article are adapted from educational slides developed specifically for lay (non-clinician) adults and youth who travel annually on mission trips to Aedes endemic areas with support from a mission-driven community church in Maryland (Audain, 2013a; 2013b). The next section of the article will present an exemplar that discusses customized teaching tools about dengue fever developed for laypersons traveling for mission trips. The summary will offer recommendations for nurses to consider as they plan teaching to increase awareness about these illnesses to prevent and control outbreaks.
Arboviruses
Brief Background
Arbovirus is a descriptive term for hundreds of viruses transmitted by arthropods... Arbovirus is a descriptive term for hundreds of viruses transmitted by arthropods (e.g., mosquitoes, flies, ticks). The word arbovirus is an acronym (Arthropod-Borne virus). There are many types of arboviruses, and they share complex life cycles involving mammals or birds, humans, and mosquitoes (Fauci & Morens, 2016). Nurses can become more knowledgeable of mosquito-borne viruses by focusing on five commonly known arboviruses which share similar symptoms, vectors, viral families, and genus such as chikungunya fever virus (CHIKV), dengue virus (DENV), West Nile virus (WNV), yellow fever virus (YFV), and the Zika virus (ZIKAV). The Table and Figure 1 offer a comparison of these five viruses (Chin, 2000).
Table. Comparison of Mosquito-Borne Viruses (Chin, 2000)
|
Name of Virus |
Name of Virus Family, Genus |
Vector, Aedes, Species |
Disease Syndrome |
Where Found |
|
Chikungunya |
Togaviridae, Alphavirus |
A. aegypti, |
Fever, rash, headache, nausea, vomiting, joint pain, hemorrhage rare, asymptomatic |
Africa, South East Asia, Philippines |
|
Dengue 1, 2, 3, 4 |
Flaviviridae, Flavivirus |
A. aegypti, |
Fever, rash, headache, malaise, joint pain, nausea, vomiting, hemorrhagic fever, shock syndrome, asymptomatic |
Throughout the Tropics, Europe, Middle East, Croatia, Italy, Norway, USA |
|
West Nile Virus |
Flaviviridae, Flavivirus |
A. aegypti, |
Fever, rash, malaise, joint pain, nausea, vomiting, headache, encephalitis, asymptomatic |
Africa, Indian subcontinent, Middle East, Europe |
|
Yellow Fever |
Flaviviridae, Flavivirus |
A. aegypti, |
Fever, chills, headache, backache, muscle pain, nausea, vomiting, jaundice, hemorrhagic fever, asymptomatic |
Africa, South America |
|
Zika |
Flaviviridae, Flavivirus |
A. aegypti |
Fever, maculopapular rash, conjunctivitis, joint pain, headache, muscle pain, asymptomatic |
Americas, Oceania/Pacific Islands |
Figure 1. Vector Transmission
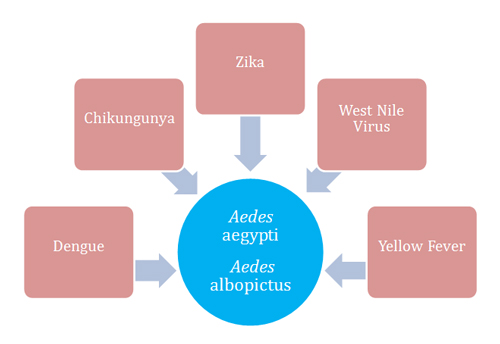
Disease control is complex and needs to involve public health education, exposure prevention, and vector control. Local and global management of mosquito-borne viruses without a vaccine or cure relies heavily on prevention and palliative treatment. Disease control is complex and needs to involve public health education, exposure prevention, and vector control.
In the current environment, everyone must consistently take protective measures, whether traveling through or living in an endemic area. Mosquito-borne viruses are receiving increased public attention; they are perceived as a rapidly growing public health threat to the global community as vector mosquitos increasingly adapt and thrive in urban environments (Mayer, Tesh, & Vasilakis, 2016). The recent emergence of Zika has especially brought increased awareness to the need for personal protection against mosquito-borne viruses. Considering dengue fever alone, almost half of the global population are at risk of infection, since there are an estimated 3.6 billion people living in endemic urban tropical and subtropical regions, including Europe and United States (Gubler, 2012). Dengue is considered a persistent global viral threat transmitted mostly by two mosquitos, Aedes aegypti and Aedes albopictus (Mayer et al., 2016). The A. aegypti species and A. albopictus are two main vectors spreading worldwide due to international trade and travel (Mayer et al., 2016; Medlock et al., 2016).
Mosquito-borne illnesses have spread throughout the entire globe due to mosquito migration and vector ability to adapt and thrive in various climates and conditions. Mosquito-borne illnesses have spread throughout the entire globe due to mosquito migration and vector ability to adapt and thrive in various climates and conditions. In the 1970s, United States government interventions resulted in control of mosquitos and mosquito-borne viruses in the southeastern United States and Caribbean. There was a sense among many scientists that dengue was eradicated and justified a near complete stop of aggressive (chemical) vector control. The worldwide dengue resurgence and the emergence of dengue hemorrhagic fever (DHF) is linked to ecologic disruption; population growth; uncontrolled urbanization; inconsistent mosquito control; increased international air travel; and lack or cessation of resources in healthcare and breeding site reduction (Gubler, 1998; Medlock et al., 2016). By the mid-1980s, American resurgence of imported dengue virus resulted in newly identified mosquito strains and serotypes (Mayer, Tesh, & Vasilakis, 2016). The spread of chikungunya and Zika virus illness in the last three years provide the most recent examples of this rapid global expansion pattern (Fauci & Morens, 2016; Imperato, 2016; Mayer et al., 2016).
Vector Ecology
A vector is an organism that does not cause disease itself but carries disease pathogens from one host to another. A vector is an organism that does not cause disease itself but carries disease pathogens from one host to another (U.S. Environmental Protection Agency [U.S. EPA], 2016). For example, species of mosquitos serve as vectors for diseases with no cure like dengue, zika and west nile virus. Humans and mosquitoes are both considered to be the viruses hosts. Ecology is the relationship between the environment and living things or the study of such relationships (U.S. EPA, 2016). Vector ecology is a term that describes the relationship between vector organisism and the environment (Institute of Medicine, 2008).
Mosquitos. Mosquitos are a type of arthropod. They are a cold-blooded (ectothermic) species with an exoskeleton made of chitin. Arthropods include ticks, triatomine bugs, sandflies, and blackflies. They are sensitive to climatic factors and temperature. (European Center for Disease Prevention and Contol, 2016). Arthropods are also called vectors as they transmit disease thru a virally infected bite during a blood meal. Vector-borne diseases are infections transmitted by the bite of the infected arthropod species.
For more than 20 years, endemic dengue was rare in the Americas due to an aggressive government-sponsored Aedes aegypti vector eradication program. This intervention ended in the early 1970s (Gubler, 1998). Depending on the geographical area, there are a number of Aedes sub-species which act as a vector in the transmission of DENV. Aedes albopictus (known as the Asian Tiger mosquito) and other Aedes sub-species such as A. africanus, and A. luteocephalus transmit chikungunya and dengue (Chen & Wilson, 2010; Medlock et al., 2016).
The female Aedes aegypti is an efficient, thriving, and invasive vector capable of spreading many arboviruses... The female Aedes aegypti is an efficient, thriving, and invasive vector capable of spreading many arboviruses, such as chikungunya fever virus (CHK), dengue virus (DENV), West Nile virus (WNV), and yellow fever virus (YFV). Scientists now suggest that the Zika virus (ZIKAV) should also be included in this grouping. Experts report that A. aegypti originated in Africa (Amarasinghe, Kuritsky, Letson, & Margolis, 2011). The A. aegypti vector has a voracious appetite, feeding exclusively on humans when in urban areas. Breeding occurs primarily in any water-holding containers and around buildings (Fauci & Morens, 2016; Mayer et al., 2016; Medlock et al., 2016).
Figure 2. Comparison of Aedes albopictus and Aedes aegypti Vectors
|
Aedes aegypti vector |
Aedes albopictus vecto |
 |
 |
|
|
(Audain, 2013a; Centers for Disease Control, 2016f; Centers for Disease Control, n.d.)
Symptoms of arbovirus infection generally occur 3 to 15 days after exposure to the virus and last 3 or 4 days. Viruses. Symptoms of arbovirus infection generally occur 3 to 15 days after exposure to the virus and last 3 or 4 days (ECDC, 2016). The CHIKV is a member of the genus Alphavirus, family Togaviridae, historically known to originate in the sub-Saharan African jungles, and primarily a zoonotic virus found in non-human transmission cycle. Global expansion and travel have contributed significantly to the emergence of CHIKV in the coastal areas of Kenya, Asia, Indian Ocean and Mediterranean Europe (Volk et al., 2010).
Another example of the complexity of arthropod-borne viruses is the dengue virus (DENV). DENV is a single-stranded RNA virus made up of four distinct strains or serotypes classified according to biological and immunological criteria (Rogers, Wilson, Hay, & Graham, 2006; WHO, 2009). Dengue belongs to the Flaviviridae family, a genus flavivirus, and is closely related to other infections that include West Nile virus and yellow fever (Gobbi et al., 2012).
Immunity to dengue virus can be complicated. The time to reach herd immunity in local populations can take much longer because there are four types of dengue viruses that are closely related: DENV-1, DENV-2, DENV-3, and DENV-4. When one type of dengue virus infects one person, there is lifelong immunity against that particular serotype, but very little cross-immunity to other serotypes (WHO, 2012). Evidence has suggested that sequential infection with a different serotype of dengue virus increases the risk of more severe (hemorrhagic) disease resulting in shock syndrome and death (WHO, 2016a, 2009). Each serotype of dengue may be mosquito vector specific depending on the geography. Serologic tests and diagnosis of flaviviruses are costly and time-consuming. There is no vaccine or effective anti-viral drug.
The ZIKV is an arbovirus of the Flaviviriade family, genus Flavivirus, that is rapidly expanding globally into new geographic areas (Mayer, Tesh, & Vasilakis, 2016). There is also growing evidence that a second mode of transmission of the ZIKV is via semen and the question of exposure duration remains unknown (Imperato, 2016). However, many scientists agree (Imperato, 2016) that herd immunity in local populations will eventually bring the Zika epidemic under control, as with many communicable diseases.
Pathogen Transmission
Multiple modes of transmission exist in DENV and ZIKV infected areas and include humans, non-human primates, vertebrates, and mosquitoes. Infection reservoirs in vertebrates can remain undetected, with sporadic “spillover” of infection from animals to humans. This results in localized outbreaks with cycles of continuous or discontinuous exposures. There are historical cases of DENV outbreaks in Asia and Africa where sylvatic, endemic DENV has spilled over into the human population (Mayer et al., 2016). Further complicating control of both the disease and vector transmission, there are reports of DENV transmission as infected human-to-naïve (unexposed) mosquito-to-naïve (unexposed) human (Audain, 2013b). Importation of DENV by a human carrier into a naïve population of both humans and mosquitoes has expanded infected regions well into the temperate climate zone where the disease was not present. The same host and transmission modes can be found in the transmission of ZIKV, prompting a resurgence of previously effective vector control measures (e.g., mosquito repellants, insectisicides, and clothing barriers) in the effort to control both diseases.
Over many years, the arbovirus-infected mosquito has become well adapted to breeding in human water sources while the arbovirus itself has adapted to infect humans. Over many years, the arbovirus-infected mosquito has become well adapted to breeding in human water sources while the arbovirus itself has adapted to infect humans (Fauci & Morens, 2016). When a susceptible female A. aegypti mosquito takes a blood meal (or bites) a person infected with DENV the mosquito becomes infected with that person’s virus. The virus then binds to receptors in the gut of the mosquito, where it can replicate. New progeny virus borne in the mosquito gut are then shed into the mosquito’s circulatory system and it is disseminated to other tissues, including the salivary glands. At this point, when the female mosquito bites another person, transmitted virus infects this new person. Another mosquito then bites this newly infected person, restarting the cycle of transmission, as illustrated in Figure 3. (Carrington & Simmons, 2014). Given the continual nature of this cycle, the larger the mosquito population with access to uninfected humans, the greater the spread of DENV or other arboviral disesases will be.
Figure 3. Continual Cycle of Transmission
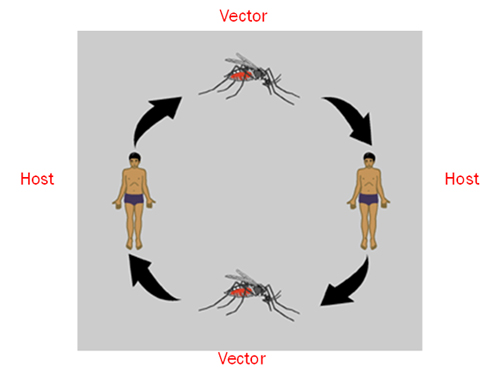
Clinical Manifestations
...with some arboviral illnesses, many infected people are asymptomatic and remain undiagnosed. There are many overlapping clinical symptoms in chikungunya, dengue, West Nile, yellow fever, and Zika viruses primarily because they share the same aedes vectors and transmission cycle. This results in challenges for definitive diagnosis on the basis of a clinical presentation alone and can cause a given diagnosis to be overlooked. Also, with some arboviral illnesses, many infected people are asymptomatic and remain undiagnosed (Whitehorn & Simmons, 2011). If these infections are overlooked, nurses engaging with these individuals miss the opportunity to teach or reinforce mosquito-borne illness prevention measures to protect them and others from future infections. This section provides a brief summary of clinical manifestations these five viruses.
Chikungunya. Chikungunya fever in an adult can occur 3 to 7 days after the incubation period. Symptoms are fever, headache, joint pain, muscle pain, joint swelling, or rash. (CDC, 2016a).
Dengue fever. Dengue fever in an adult can occur 4 to 7 days after the incubation period. The 2011 WHO case definition (Amarasinghe et al., 2011) for a suspected dengue infection is a patient with high fever and two of any of the following signs or symptoms: headache; retro-orbital pain; myalgia; arthralgia; rash; bleeding manifestations; leukopenia; and platelet count and hematocrit rising up to 10 percent above normal levels. The clinical manifestation of dengue in children can present differently from adults with primary symptoms of cough, vomiting, and abdominal pain (Whitehorn & Simmons, 2011).
... in many cases diagnostic tests or test results may be unavailable or providers are unable to distinguish between one viral illness and another. West Nile. West Nile virus fever in an adult can occur 4 to 7 days after the incubation period. Symptoms are fever, headache, body aches, joint pains, vomiting, diarrhea, or rash. Serious neurologic illnesses (e.g., encephalitis, meningitis) may occur rarely (CDC, 2016).
Yellow fever. Acute yellow fever in an adult can occur 3 to 6 days after the incubation period and last with 3 to 4 days of acute viral hemorrhagic disease. Symptoms of acute yellow fever are fever, headache, jaundice, muscle pain, nausea, vomiting, and fatigue. Fifteen percent of people exposed exhibit a more toxic phase within 24 hours. (CDC, 2016)
Zika. Zika fever in an adult may occur 4 to 7 days after the incubation period. Symptoms are broad and similar to dengue and many other arboviruses of the Flaviviriade family, genus Flavivirus viral disease. Clinical manifestations include headache; acute onset of fever with maculopapular rash; arthralgia; conjunctivitis; retro-orbital pain; myalgia; and vomiting. Many people are asymptomatic. There have been reports of the virus found in utero in pregnant women and in seminal fluid resulting in male-to-female sexual transmission events (Imperato, 2016). Careful interpretation of the clinical manifestations of pregnant women with seek infection is critical because consequences to unborn children are extremely serious (e.g. microcephaly). Another clinical phenomenon is the reporting of Guillain-Barre syndrome in patients suspected to have had Zika infection (CDC, 2016; Mayer et al., 2016).
Making a Diagnosis
Diagnosis and laboratory diagnostic tests. Preliminary diagnosis for mosquito-borne viruses is based on the patient’s clinical features; places and dates of travel; and activities (CDC, 2016). The choice of direct or indirect diagnostic tests depends on availability of testing; purpose of testing; and stage of disease (WHO, 2009). Laboratory diagnosis is generally accomplished by testing serum or plasma to detect virus, viral nucleic acid, or virus-specific immunoglobulin M and neutralizing antibodies (CDC, 2016). However, in many cases diagnostic tests or test results may be unavailable or providers are unable to distinguish between one viral illness and another.
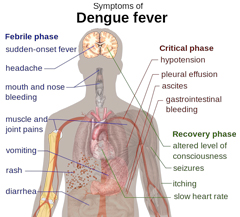
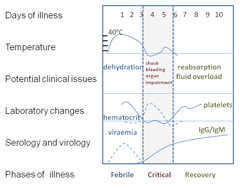
Two important ways to identify these illnesses are to obtain a good patient travel history and to identify and compare the common clinical manifestations of arboviral illnesses. Dengue fever example. Two important ways to identify these illnesses are to obtain a good patient travel history and to identify and compare the common clinical manifestations of arboviral illnesses. A person can be bitten by an infected Aedes vector four separate times, each with a different serotype of DENV, and the human host would develop symptoms and immunity with each exposure (Amarasinghe et al., 2011). Travelers in and out of areas endemic with different viral serotypes are at greater risk of morbidity and mortality with each exposure (Mirzalian, Durham & Hess, 2010), thus the importance of a thorough history. Figure 4 offers typical information that by be helpful to patients (left) and providers (left and right) to determine the exact type of arbovirus infection. Information in the figure might also be helpful to generate conversation to teach individuals why and how to protect themselves to reduce the spread of disease
Figure 4. Clinical Manifestation of Dengue Fever Example
|
How Do I Know I Have Dengue? |
|
|
|
(Audain, 2013a; Wikimedia Commons, 2016a, 2016b; WHO, 2009)
Prevention and Vector Control
Prevention and vector control requires medical intervention if possible; mosquito control; and education and training for providers and patients. Informed nurses, who interact with patients for direct care, can offer leadership in the effort to raise awareness and support prevention.
Limited medical interventions. For many arboviral illnesses there is no vaccine or specific drug treatment available. Therefore, vector control through environmental means (e.g., spraying for control) and fostering behavior change that leads to sustained personal bite prevention (e.g., appropriate clothing and repellents) are the primary ways to reduce and control vector-borne illnesses (WHO, 2009).
Mosquito control. Travelers have an integral role in global vector control. Awareness (or lack thereof) of dengue and other arboviral illnesses has been documented in published reports of diagnosis in travelers who have returned home (Mayer et al., 2016). It is important to have awareness of current and potential threats related to travel in identified areas of risk.
Personal self-management measures are critical for protection against mosquito exposure and reduction of biting activity. Personal self-management measures are critical for protection against mosquito exposure and reduction of biting activity. This can be achieved by using clothing that minimizes skin exposure; repellents which contain DEET; insecticide-treated mosquito nets; household insecticide aerosol products; household fixtures (e.g., door screens, indoor air-conditioning); and emptying outside cans or garbage containers with standing water (Gubler, 1998; WHO, 2009).
Education and training. Education and training about prevention is important for those who travel to or reside in endemic areas to improve threat recognition and awareness of risk of infection, and to reduce transmission. Education should be included in nursing and medical school curricula; provided to national level committees considering mosquito borne illnesses; offered to all levels of staff on medical mission trips; and disseminated to the public via mass media workshops designed to educate but not alarm (Wilder-Smith et al., 2012). Effective public awareness is achieved by distributing printed information about illnesses and warning signs via community workshops and seminars.
The discussion above summarizes basic information about mosquito-borne illnesses that can be helpful to nurses as they plan and implement health education activities to teach individuals and communities about disease prevention and control. The next section discusses educational activities that evolved from the content above, originally designed to educate individuals at a local level preparing for mission trip, but also appropriate in other contexts.
Exemplar: Customized Teaching Tools About Dengue Fever
In an effort to create useful educational materials for persons who might need or be interested in information about prevention of mosquito-borne illnesses, the first author (Audain) will describe several options developed primarily for those traveling on mission trips. Each of these considers awareness and prevention about dengue fever. Each was designed in a simple, plain language format that includes, when possible, the rationale to support the recommended preventive behaviors. The exemplar demonstrates a process of approaching the topic at a local level to determine content and usefulness, followed by use of easily accessible technology to reach (in English) a global level audience.
Pilot presentation. A pilot project was developed for adults and youth who attend a community church in Maryland to prepare them for a mission trip in Africa (Audain, 2013a; 2013b). The first project included two presentations about dengue fever using PowerPoint slides to the church’s mission council meeting, and to church members.
Educational brochure. In response to the requests from elderly and youth church members in the pilot group, the next step was creation of an educational brochure (Audain, 2014). Audain forged a partnership with the mission volunteer community and designed a comprehensive brochure, Dengue Awareness and Prevention for Mission Trips (2014). To ensure that a brochure would be useful and customized to meet the needs of non-clinicians who travel, the presenter designed simple surveys for participants to complete before and after each presentation. Responses indicated that participants had learned from the content presented using the PowerPoint slides. A customized, 4-sided brochure about prevention and awareness was developed (Audain, 2014) with the help of a graphic designer. Information on the brochure provides specific information about dengue awareness and prevention for mission trips, including content about what dengue is and the types and phases; the human host of dengue; who is at risk; prevention; symptoms; treatment; and a visual map indicating the geographic location and severity of globally affected areas. The brochure was evaluated for readability by a diverse group of greater than 20 potential readers including academic colleagues, healthcare doctoral students, and laypersons (see Figure 5 for the complete brochure). The brochure was eventually distributed to over 3,000 church members (Audain, 2014).
Figure 5. Educational Brochure


(Audain, 2014; author holds copyright)
eLearning pdf tool. The two pilot dengue prevention presentations and the brochure were well received at the community church. However, the traveling church members would be in an endemic area. It was still unclear if this effort would be enough to influence behavioral change among the participants, who would face an environment that required consistent protective measures. Audain (2013a; 2013b; 2014) continued work to offer dengue fever awareness and prevention. The next phase of development was an educational eLearning tool on dengue awareness and prevention for non-medical and medical persons in mission-focused church and Non-Governmental Organizations. This tool is available as a PDF document.
The community knowledge sharing website wikiHow (n.d.a) was useful to design a virtual teaching tool that could reach many people. wikiHow tool. The community knowledge sharing website wikiHow (n.d.a) was useful to design a virtual teaching tool that could reach many people. WikiHow is a website open to authors interested in sharing their knowledge to help others learn. It is universal in 17 languages, a free basic service in 33 countries, and an open source software in which the content is Creative Commons licensed (wikiHow, n.d.c).
The first author (Audain) initiated and first published a dengue prevention and awareness wikiHow, wikiHow to Avoid Getting Dengue Fever on a Mission Trip (wikiHow, n.d.b) on July 22, 2013. The goal of this teaching tool was to reach lay individuals who go on mission trips on a much wider scale than in a local settings such as the community church.
The virtual teaching tool house on wikiHow (n.d.b) has three main parts: understanding the disease, being aware, and avoiding mosquitoes. Each part includes colorful graphics appropriate to the topic to engage viewers and simple, plain language information listed in short sentences and/or bullets. Simple rationale is also provided to support recommendations. For example, in the part Avoiding Mosquitoes, the first step listed is to understand the mosquitoes biting and breeding routine, and the rationale states that this will help to avoid them. Following this are specific steps related to the routine. This tool was evaluated for face validity and readability in a method similar to the educational brochure previously discussed.
The use of the wikiHow tool opened the availability of this information on a global level to anyone interested. Between initial publication on July 22, 2013 and late December 2016, the page had almost 6,500 views. It also had 12 votes related to its helpfulness, and 11 of the viewers who voted indicated that the site was helpful. The structure of a wiki allows for community editing; this page lists seven co-authors, indicating engagement and editing from readers.
Summary and Recommendations
Increasing understanding about why preventive measures are important may help persons at risk to take protective steps consistently. Nurses are excellent health and community educators and are known for their personal approach. Using a one on one communication style, they share complex scientific, medical, and public health information, and assess individual understanding. The art of effectively teaching patients and communities can lead to changing behavior from better understanding. One example of this is awareness and prevention for mosquito-borne illnesses. Increasing understanding about why preventive measures are important may help persons at risk to take protective steps consistently. This article has briefly reviewed five mosquito-borne illnesses becoming increasingly common due in part to the ease of world travel for many, and an exemplar of education related materials for one of them, dengue fever.
Opportunities to provide education range from face-to-face presentations in local settings to globally available content using current technology. Important considerations recommended by the authors for nurses who provide education about these illnesses include:
- Use plain, descriptive language to provide information about the illness. Keep it simple.
- Include graphics to increase visual interest and demonstrate concepts.
- Whenever possible, provide a rationale to help readers understand not just what they should do and how to do it, but why it is important.
- Provide context for readers. Help them to understand how preventive measures can help not only themselves, but also others. Conversely, help them to understand how failing to take these measures can also impact others.
- Explore multiple ways to provide information to take advantage of opportunities to increase exposure to your content geographically, and also to help readers access content in ways convenient for them (e.g., brochure, smart phone).
Around the world, nurses have the opportunity to influence changes in behavior. With the increase in emerging global health concerns, including those of mosquito-borne illnesses (Bouri et al., 2012; CDC, 2016a, 2016b; Van Dodewaard & Richards, 2015), there is a significant need for nurses to use teaching skills to increase understanding for persons at risk for these and other illnesses (CDC, 2016c, 2016d, 2016e).
Note
This article reflects the views of the authors and should not be construed to represent the U.S. Food and Drug Administration views or policies.
Authors
Gettie Audain, DHSc, MPH, BSN, RN, APHN-BC
Email: audget@yahoo.com
Dr. Gettie Audain is a nurse officer and Captain in the U.S. Public Health Service Commissioned Corps since 2002. Her nursing career spans nearly 30 years caring for culturally diverse populations in urban settings. Her clinical experience includes public health nursing with clinical expertise in emergency, disaster care, hemodialysis, gastroenterology, HIV/AIDS, and public health policy. CAPT Audain's nursing foundation began at Jackson Memorial Hospital School of Nursing, Diploma program, and then eight years at the hospital. She earned her Bachelor of Science in Nursing degree at Florida International University, Miami, FL, and a Master of Public Health degree from Walden University, Minneapolis, Minnesota. CAPT Audain completed her Doctor of Health Science degree with a concentration in Global Health from Nova Southeastern University, in Fort Lauderdale, Florida and received her Advanced Public Health Nursing Board Certification from the American Nursing Credentialing Center.
Carmen Maher, MA, BSN, RN, RAC
Email: carmah@ymail.com
RADM Carmen Maher is a nurse officer and Assistant Surgeon General in the U.S. Public Health Service Commissioned Corps. RADM Maher began her nursing career in 1993 as an Ensign in the U.S. Navy, assigned to the National Naval Medical Center in Bethesda, Maryland. She has more than 20 years of experience in nursing, medical products regulations, clinical trials/medical product development, public health, and emergency response. RADM Maher is recognized as a national expert in Chemical, Biological, Radiological, Nuclear (CBRN) threats, Emerging Infectious Diseases (EID), & Global Health Security (GHS). She works in collaboration with U.S. government agencies and other relevant stakeholders to define and prioritize requirements for medical countermeasures (MCMs) to respond to public health emergencies, coordinate research for evaluating MCMs, set strategies for deployment and use of MCMs, and facilitate access to MCMs during public health emergencies. RADM Maher earned an associate’s degree and BSN from the University of Puerto Rico. She earned an M.A. in National Security and Strategic Studies with highest distinction from the U.S. Naval War College in Rhode Island, and holds a Regulatory Affairs Certification in U.S. healthcare product regulations.
Centers for Disease Control and Prevention. (n.d.). Aedes aegypti. Aedes albopictus. Retrieved from https://www.cdc.gov/dengue/resources/30Jan2012/comparisondenguevectors.pdf
wikiHow to do anything. (n.d.a). We’re trying to help everyone on the planet how to do anything. Join us. Retrieved from http://www.wikihow.com/Main-Page
References
Amarasinghe, A., Kuritsky, J. N., Letson, G. W., & Margolis, H. S. (2011). Dengue virus infection in Africa. Emerging Infectious Diseases, 17(8), 1349-1354. doi:10.3201/eid1708.101515
Audain, G. (2013a, March 10). Dengue awareness and prevention for mission trips to Africa [Power Point Slides]. Nova Southeastern University. Presentation to Immanual’s Church Mission Council Meeting on March 10, 2013.
Audain, G. (2013b). Dengue awareness project for a church-based medical mission trip to Africa. [Doctoral Practicum Paper] Nova Southeastern University.
Audain, G. (2014). Dengue awareness and prevention for mission trips. [Unpublished Brochure].
Bouri, N., Sell, T. K., Franco, C., Adalja, A. A., Henderson, D. A., & Hynes, N. A. (2012). Return of epidemic dengue in the United States: Implications for the public health practitioner. Public Health Reports, 127(3), 259–266.
Carrington, L.B., & Simmons, C. P. (2014). Human to mosquito transmission of dengue viruses. Frontiers in Immunology. doi:10.3389/fmmu.2014.00290
Centers for Disease Control and Prevention. (2016a). Chikungunya virus in the United States. Retrieved from http://www.cdc.gov/chikungunya/geo/united-states.html
Centers for Disease Control and Prevention. (2016b). Chikungunya Virus: Prevention. Retrieved from http://www.cdc.gov/chikungunya/prevention/index.html
Centers for Disease Control and Prevention. (2016c). Prevention: How to reduce your risk of dengue infection. Retrieved from http://wwwnc.cdc.gov/travel
Centers for Disease Control and Prevention. (2016d). Zika Virus: At-a-glance. Retrieved from https://www.cdc.gov/zika/
Centers for Disease Control and Prevention. (2016e). Zika Virus: Prevention. Retrieved from http://www.cdc.gov/zika/prevention/index.html
Centers for Disease Control and Prevention. (2016f). Denague: Entomology & ecology. Retrieved from https://www.cdc.gov/Dengue/entomologyEcology/index.html
Centers for Disease Control and Prevention. (n.d.). Aedes aegypti. Aedes albopictus. Retrieved from https://www.cdc.gov/dengue/resources/30Jan2012/comparisondenguevectors.pdf
Chen, L. H., & Wilson, M. E. (2010). Dengue and chikungunya infections in travelers. Current Opinion in Infectious Diseases, 23(5), 438-444. doi:10.1097/QCO.0b013e32833c1d16
Chin, J. (Ed.). (2000). Communicable diseases manual (17th ed.). Washington, DC: American Public Health Association
European Center for Disease Prevention and Control. (2017). Climate change in Europe. Retrieved from http://ecdc.europa.eu/en/healthtopics/climate_change/pages/index.aspx
Fauci, S. A., & Morens, M. D. (2016). Zika virus in the Americas – Yet another arbovirus threat. [Perspective]. The New England Journal of Medicine, 374(7), 601-603. doi:10.1056/NEJMp1600297
Fogarty International Center. (2016). HHS makes progress on Zika, yellow fever vaccines. Global Health Matters, Sept/Oct 2016, 2. Retrieved from https://www.fic.nih.gov/News/GlobalHealthMatters/september-october-2016/Documents/fogarty-nih-global-health-matters-newsletter-september-october-2016.pdf
Gobbi, F., Barzon, L., Capelli, G., Angheben, A., Pacenti, M., Napoletano, G., . . . the Vento Summer Fever Study Group. (2012). Surveillance for west nile, dengue, and chikungunya virus infections, Vento Region, Italy, 2010. Emerging Infectious Diseases, 18(4), 671-673. doi:10.3201/eid1804.110753
Gubler, D. J. (1998). Dengue and dengue hemorrhagic fever. Clinical Microbiology Reviews, 11(3), 480-496. Retrieved from: http://cmr.asm.org/content/11/3/480.full
Gubler, D. J. (2012). The economic burden of dengue [Editorial]. The American Journal of Tropical Medicine and Hygiene, 86(5), 743-744. doi:10.4269/ajtmh.2010.12-0157
Imperato, P.J. (2016). The Convergence of a Virus, Mosquitoes, and Human Travel in Globalizing the Zika Epidemic. Journal of Community Health, 41(3), 674-679. doi:10.1007/s10900-016-0177-7
Institute of Medicine (US) Forum on Microbial Threats. (2008). Vector-borne diseases. Washinton, DC: National Academies Press. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK52939/
Kenyon College Department of Biology. (n.d.) Dengue transmission. Retreived from Microbwiki: https://microbewiki.kenyon.edu/index.php/Dengue_transmission
Mayer, S.V., Tesh, R.B., & Vasilakis N. (2016). The emergence of arthropod-borne viral diseases: A global prospective on dengue, chikungunya and zika fevers. Acta Tropica. 166, 155-163. doi: 10.1016/j.actatropica.2016.11.020.
Medlock, J. M., Hansford, K. M., Schaffner, F., Versteirt, V., Hendrickx, G., Zeller, H., & Bortel, W. V. (2012). A review of the invasive mosquitoes in Europe: Ecology, public health risks, and control options. Vector Borne and Zoonotic Diseases, 12(6), 435–447. doi:10.1089/vbz.2011.0814
Mirzalian, E., Durham, M. J., & Hess, K. (2010). Mosquito-borne illness in travelers: A review of risk and prevention. Pharmacotherapy, 30(10), 1031-1043.
National Institute of Allergy and Infectious Diseases. (2016). Zika virus vaccines. Retrieved from https://www.niaid.nih.gov/diseases-conditions/zika-vaccines
National Institute of Allergy and Infectious Diseases. (2015). NIH-funded vaccine for West Nile virus enters human clinical trials [Press Release]. Retrieved from https://www.nih.gov/news-events/news-releases/nih-funded-vaccine-west-nile-virus-enters-human-clinical-trials
Prima Quality Media. (2014). Dengue virus transmission cycle. Retrieved from http://archive.is/RGZPJ
Rogers, D. J., Wilson, A. J., Hay, S. I., & Graham, A. J. (2006). The global distribution of yellow fever and dengue. Advances in Parasitology, 62, 181-220. doi:10.1016/S0065-308X(05)62006-4
Roos, R. (2015, March 2). Chikungunya vaccine looks promising in phase 1 trial. Center for Infectious Disease Research and Policy
U.S. Environmental Protection Agency. (2016) EPA terms of environment dictionary INDEX. Retreived from http://www.ecologydictionary.org/EPA-Terms-of-Environment-Dictionary/
Van Dodewaard, C. A. M., & Richards, S. L. (2015). Trends in dengue cases imported into the United States from Pan America 2001–2012. Environmental Health Insights, 9, 33–40. doi:10.4137/EHI.S32833
Whitehorn, J., & Simmons, C. P. (2011). The pathogenesis of dengue [Review]. Vaccine, (29), 7221-7228. doi:10.1016/j.vaccine.2011.07.022
Wikimedia Commons. (2016a). File: Dengue fever syptoms.svg. Retrieved from https://commons.wikimedia.org/wiki/File:Dengue_fever_symptoms.svg
Wikimedia Commons. (2016b). File: Course of Dengue illness.png. Retrieve from https://commons.wikimedia.org/wiki/File:Course_of_Dengue_illness.png
wikiHow to do anything. (n.d.a). We’re trying to help everyone on the planet how to do anything. Join us. Retrieved from http://www.wikihow.com/Main-Page
wikiHow to do anything. (n.d.b). wikiHow to avoid getting dengue fever on a mission trip. Retrieved from http://www.wikihow.com/Avoid-Getting-Dengue-Fever-on-a-Mission-Trip
wikiHow to do anything. (n.d.c). WikiHow: Mission. Retrieved from https://www.wikihow.com/wikiHow:Mission
Wilder-Smith, A., Renhorn, K-E., Tissera, H., Bakar, S. A., Alphey, L., Kittayapong, P., Lindsay, S., . . . Gubler, D. (2012). Dengue tools: Innovative tools and strategies for the surveillance and control of dengue. Global Health Action, 5, 17273. doi:10.3402/gha.v5i0.17273
Woerner, A. (2013, November 25). Dengue fever: Why it’s becoming more common in the U.S. and what Americans should know. FoxNews Health, Outbreaks. Retrieved from: http://www.foxnews.com/health/2013/11/25/dengue-fever-why-its-becoming-more-common-in-us-and-what-americans-should-know.html
World Health Organization. (2016a). Dengue and severe dengue. Retrieved from http://www.who.int/mediacentre/factsheets/fs117/en/
World Health Organization. (2016b). Dengue vaccine research. Retrieved from http://www.who.int/immunization/research/development/dengue_vaccines/en/
World Health Organization. (2012). Global report for research on infectious diseases of poverty. Geneva, Switzerland:Author. Retrieved from: http://www.who.int/tdr/stewardship/global_report/en/
World Health Organization. (2009). Dengue: guidelines for diagnosis, treatment, prevention and control [New edition]. Geneva, Switzerland: Author. Retrieved from: http://whqlibdoc.who.int/publications/2009/9789241547871.eng.pdf

